The jaw on the left hurts. Jaw hurts when jawbone or mouth opening: can do? Complications of inflammation of the heart
What to do in this case, the doctor will tell. This condition significantly affects the quality of life, such patients turn to surgeons, dentists, traumatologists for treatment. The doctor can help immediately if there has been a dislocation, or the treatment may be delayed for a long time.
The causes of the symptoms of pain are as follows:
- The presence of a fracture in the bone structure that arose as a result of a direct blow to the jaw, in an accident, in an accident. In all these moments, a mechanical effect on the jaw bones occurs. In this case, the upper and lower jaws can be broken individually or together. A fracture is direct or reflected, single or multiple, with the presence of bone fragments, unbiased, open and closed. Symptoms of a fracture are manifested by soreness in the organ, swelling appears, and motor functions are impaired.
- Infection with an infectious disease leading to osteomyelitis. Pathology is manifested by the inflammatory process in all areas of the bones. The infection enters the outbreak either through blood or through infection of a pocket located between the tooth and gum. The most common causative agents are staphylococcal bacillus, anaerobes, streptococci. If the pain in the jaw joint is pulsating, accompanied by a headache and fever, then the likelihood of developing osteomyelitis is high. The treatment of the disease consists in detecting the affected tooth and the gums reddened around it, opening the focus to remove pus. Then, for several days, manipulations are carried out for its outflow, a course of antibiotics with symptomatic therapy is prescribed. In such patients, in the general blood test, a shift of the leukocyte formula to the left and an increased erythrocyte sedimentation rate are observed. The patient's condition can be mild, moderate and severe.
- Odontogenic factor - when pain in the joint, in the jaw occurs after the appearance of pathology of the teeth and gums. Such conditions include caries, which has spread to the deep parts of the tooth with a nerve, with damage to the pulp, suppuration of tissues around the teeth. Painful sensations intensify at night, are pulsating in nature. The patient feels pain in the root of the tooth, the symptoms spread to the corresponding jaw. The doctor, upon detection of an affected tooth, removes it, carries out the sanation of the focus. However, often the consequences of this disease affect the trigeminal nerve of the face, the damage is characterized by a feeling of numbness of the lips, a decrease in chewing muscle tone.
- Inflammation of the arteries of the face - a pathological condition, accompanied by a burning sensation, spreads to the chin, jaw joint to the lips and nose. In some cases, the pathology captures wider areas of the face, reaching the corners of the eyes. The disease is diagnosed by a special sign - the pain is localized at the place of inflection of the facial artery in the region of the lower jaw.
- Functional disorders of the jaw and temple joint. In this case, the jaw joint hurts along with the temple, cheek and forehead. The patient is not able to open his mouth, with the slightest movement there is a click. The causes of violations can be an incorrect bite or the development of inflammation in this area, myofascial syndrome in the masticatory muscles, the occurrence of osteoarthritis in the joint. Therefore, when the question arises why the jaw hurts, it is necessary to exclude the connection of pain with the joint. To do this, you should consult a doctor, undergo a diagnosis and begin proper treatment.
- Inflammatory diseases of the cranial nerves (cranial nerves) can cause pain. Most often, this condition is observed with trigeminal neuralgia, while the pain is burning in nature, manifested by sudden attacks. The pain is more pronounced directly in those areas where inflammation of a certain branch of the nerve is expressed. Characteristic for this ailment is the lack of clinical manifestations in the evening and night periods. The lower jaw is not affected, the localization of pain is spread only at the location of the branches.
- With inflammation of the upper laryngeal nerve, an unpleasant sensation occurs in the larynx, thyroid gland and under the tongue. The spread of pain is wide enough: from the face and ear to the shoulders and chest. In addition, the patient is concerned about coughing, hiccups, and excessive salivation. Pain is provoked by swallowing movements, blowing your nose, coughing, and head movements. Some groups of drugs are used for therapy, local anesthesia is performed, in rare cases, the nerve itself is cut.
- The jaw joints sometimes hurt with neuralgia of the glossopharyngeal nerve. Pain can spread to all areas of the face, ears, and even tonsils. To reduce discomfort, the patient bends his head in the direction of pain. If you press on the mandibular angle, pain sensations intensify.
- With the inflammatory process in the ear node of a person, severe burning pains of a paroxysmal character are tormented. The duration of each attack is about an hour. The pain extends to the jaw and teeth. The Eustachian tube contracts, as a result of these cramps in the ears there are clicks. Eating hot or cold food can provoke or intensify soreness. To correctly diagnose this nosology, use the method of pressing fingers on the area between the mandibular joint and the external auditory canal. In this case, unpleasant symptoms intensify.
- Migraine. Such a condition in some situations may be accompanied by paroxysmal pain, lasting several hours in a row. The sensation spreads to the upper jaw with the capture of the oral cavity and ear. Then it gradually “spreads” all over the face. If you press on the branching site of the external carotid artery, the signs intensify. The same symptom is observed with the tumor process, with a layered carotid artery and with inflammation of the temporal joint.
- Sarcoma of bones. It is a malignant tumor of the bone, its occurrence among jaw tumors is more than 20%. With this disease, deforming changes in bone tissue occur, severe constant pain spreads from the jaws throughout the face, some areas of the face become numb.
Diagnosis of diseases
If you experience any discomfort in the area of \u200b\u200bthe lower or upper jaw, you must contact a medical institution, where the doctor will determine in which zone there is a lesion. The patient is examined by dentists, surgeons, traumatologists, otorhinolaryngologists. Next, a laboratory and instrumental examination is prescribed: a general blood test to determine the inflammatory process, an X-ray examination, with which they find the cause of the pain, and if necessary, computed tomography and MRI are performed. If the patient suspects cancer pathology, then conduct an analysis of tumor markers. If there is a suspicion of damage to the vessels of the head, an ultrasound examination with Doppler is used.

If there is pain, you should rather consult a specialist for help. However, if you cannot immediately go to a health facility at home, you can alleviate the symptoms of pain. To do this, use analgesic drugs, use cold lotions locally, try to reduce the load on the jaw, for this they use food crushed on a blender or grater. All this is a temporary nature of pain relief. In any case, qualified medical assistance is needed.
In cases of jaw joint dysfunction, anti-inflammatory drugs are used that reduce the physical load on the organ. If one or another neuralgia has become the cause of the pain, a course of conservative treatment prescribed by a doctor is carried out. With its inefficiency, surgery is performed - a nerve is dissected.
In case of vascular disorders, therapy is carried out by narrow specialists, the treatment method is conservative. The pain syndrome is eliminated by taking anesthetics to relax the muscles, injected steroids directly into the joint by injection. Hormones not only eliminate pain, but also significantly reduce swelling. However, among the serious side effects - the occurrence of osteoporosis, thinning of the bone, ultimately leading to the destruction of bone tissue. Locally widely used contrasting compresses that are applied to the joints with the mouth open. It is convenient to add an anti-inflammatory component to the compress. If the inflammation is not severe, a relaxing gymnastics of the muscles of the face is performed.
Insulating dressings on the jaw are used to treat mechanical damage to reduce stress. A gentle liquid diet is prescribed so that the patient does not chew food, but only swallows the chopped pieces.
In parallel, complex vitamins and minerals are prescribed for better bone growth. After restoration of bone structures, the patient must avoid serious stress, because relapse is possible.
Preventive actions
Prevention after diseases that have caused pain in the jaw is aimed at reducing the load on the joints, eating soft foods and taking calcium and chondroprotective drugs. In addition, it is necessary to avoid hypothermia or overheating. It is necessary to regularly visit the dentist's office, to carry out the rehabilitation of carious foci in time, and to monitor the condition of the oral cavity. If you experience any unpleasant sensations or sounds, you should immediately contact a hospital or clinic for timely treatment and to avoid complications.
When the jaw joint hurts, what to do to relieve the pain syndrome or start a thorough treatment can be found out by finding out the causes of the pain.
Some of the causes of the disease
Nowadays, there is a negative tendency for a problem to occur when the jaw joint in the temple area or lower jaw hurts, which is inherent in all age categories of people.
may be due to: 
- microtrauma;
- stress
- malocclusion;
- sharp overstrain in the muscles during chewing;
- unprofessional surgical intervention in the oral cavity;
- neglected old injuries;
- violation of the supply of blood to the cavity of bone and cartilage;
- infections.
Since articular elements are involved in its formation, which include the temporal bone and lower jaw, it is the thinning of these surfaces that is the most common cause of soreness and limited movement.
Treatment, diagnosis of this complex pathology is also difficult.
Symptoms of the manifestations of the disease
A complication of the diagnosis of lesions of the temporomandibular joint (TMJ) is accompanied by the fact that many symptoms are manifested. Due to the fact that there are no nerve endings in the jaw joint, its unhealthy state manifests itself:
- pain during pressure in the ear area;
- neck pain;
- a headache that provokes muscle, not only in the temples, but also the back of the head and shoulder blades.
 The manifestations of ear noise, crunch in the joints during opening the mouth are palpable.
The manifestations of ear noise, crunch in the joints during opening the mouth are palpable.
One of the common signs of a jaw joint disease will be the presence of some clicking in it, sometimes even unaccompanied by anxiety. Such sounds can be heard by others.
This is a clear sign of displacement and unnatural tension of the discs and muscles, which perform the function of maintaining the jaw joint when chewing products.
This can lead to blockage, in which the mandibular joint is set in an irregular manner.
Danger of serious consequences
The degree of headache and pain in the forehead is so great that it is interpreted by specialists as the one that arose as a result of migraines or brain pathologies.
Ear congestion can subsequently lead to such a result that there will be partial or complete hearing loss. It should be very serious about how quickly and intensively you need to start treatment.
In addition, such violations cause an uneven opening of the jaw, problems with wide opening of the mouth. The consequence may be grinding of teeth, provoking their increased sensitivity. The dentist will not remove it with any manipulations, and the pain will only intensify. Increased muscle tissue tension will lead to: 
- back pain
- dizziness
- sleep disturbance;
- depression
- confusion;
- disorientation;
- the state in which photophobia develops (increased sensitivity to light rays);
- the occurrence of eye pain;
- blurred vision;
- disruption in the muscles of the eye.
Analysis of diagnostic and preliminary assistance
In this case, a number of procedures aimed at providing moist heat will have a healing effect. Strengthening blood flow to the muscles of the jaw and relaxing them will allow the application of something warm. The pain will decrease and the chewing function will improve after applying a compress to the affected area. It can be replaced with a bottle of heated water, which, wrapped in a warm, damp towel, can be applied without fear of getting a burn.
Ice will relieve pain and reduce the inflammatory process. The duration of the procedure for applying ice wrapped in cloth should not reach a twenty-minute period of time. You can repeat the manipulation only after an hour. Cold signals will block the transmission of nerve information about the pain impulse to the brain.  Improving the blood supply will provide a massaging area around the one that bothers. You can resort to analgesics to reduce pain.
Improving the blood supply will provide a massaging area around the one that bothers. You can resort to analgesics to reduce pain.
Try not to open your mouth wide, there is only soft grated food, to allow the muscles to recover.
It is worth sticking to a diet. It will greatly simplify your recovery, reduce the load on the damaged joint while chewing food. The diet should be formed by cereals, kefir, juices, milk, cottage cheese.
Diagnosing such an ailment is very difficult. Often its detection occurs in the late stages of progression. The treatment is accompanied by a number of complex long difficult events aimed at recovery.
Under such circumstances, it will be most effective to use radiography, orthopantogram, electromyography, computed tomography, magnetic resonance imaging, arthroscopy. Achieving realistic results of the analysis and identifying the true causes of the disease will be facilitated by seeking advice and diagnostics from several highly qualified dentists with experience in various dental fields.
Effective Treatment Options
The result obtained by therapy will be positive if the following set of actions is observed: 
- orthodontic treatment in which the bite is corrected;
- correction of surgical errors;
- prosthetics;
- observance of physiotherapeutic procedures;
- acupuncture measures.
Physiotherapy events will be presented:
- microwave therapy;
- ultrasound therapy;
- laser therapy;
- dynamic current therapy;
- electrophoresis.
The joint splint may also be prescribed to be worn at night by the specialist you are treating. She removes myofascial pain syndrome. In addition to treatment, it is applicable for diagnostic procedures and is able to prevent abrasion of the dentition. Orthopedic measures will help to establish limiters for tearing off the oral cavity, palatine plates, special capes, bite plates. In no case should you postpone treatment measures to a later date and treat the problem without proper attention. The displaced disk provokes the restructuring of the articular surfaces, to which it is absolutely impossible to expose them. The entire joint cavity is filled with coarse connective tissue.
Preventative measures
 Protecting you from such difficulties is capable of timely elimination of the consequences of bruises. It is better to resort to qualified services spontaneous treatment. Give preference to high-tech prosthetics, correction of malocclusion.
Protecting you from such difficulties is capable of timely elimination of the consequences of bruises. It is better to resort to qualified services spontaneous treatment. Give preference to high-tech prosthetics, correction of malocclusion.
Chewing gum will also be followed by increased tension of the jaw muscles and an additional load on the extravasive force.
Sleep on the back or side will not provoke the formation of a skew that generates an excess of tension on the neck muscles and, accordingly, an additional load on the jaw joints is performed.
To clench your jaw with irritable and angry outbreaks will also negatively affect your health.
The location of the heavy bag on one shoulder with an uneven load causes asymmetry in the neck and back, accompanied by jaw pain. Periodically hanging the bag from one shoulder to another will ease the situation.
Refusing caffeinated drinks will be beneficial. Caffeine increases the effect of muscle tension.
Be attentive to yourself and then treatment will not be needed.
Any inflammation brings us a lot of suffering, and with problems with the jaw joint a person can’t eat at all. How to cope with facial pain? What is it in principle - inflammation of the jaw joint? and the reasons for this medical problem, we will discuss.
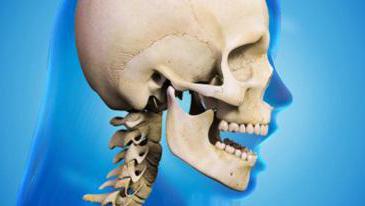
Temporomandibular joint anatomy
Temporomandibular joint (CHF) is a joint that connects the lower jaw to the temporal bone, located directly in front of the ear on each side of the head.
The joint consists of the following parts:
- head of the lower jaw;
- condyle - the head of the lower jaw entering the capsule;
- joint capsule;
- articular disc, which consists of cartilage.
- intracapsular and extracapsular ligaments.
There are two joints, and they work simultaneously. The human jaw is able to move forward, make lateral movements and move up and down. This structure allows us to chew food and talk.
If any inflammation occurs in one joint, the entire system is disrupted. Therefore, inflammation of the jaw joint requires a medical examination and proper treatment.
Inflammation is acute and chronic. Acute inflammation of the jaw joint usually occurs after an injury, loss of the condyle from the capsule or dislocation of the jaw. Chronic inflammation develops slowly, most often as a result of defects (malocclusion) or poor-quality dental work. The pain in this case is not strong, aching. Sometimes a person does not suspect the causes of this pain. It happens that inflammation is transmitted from the inner ear to the joint.
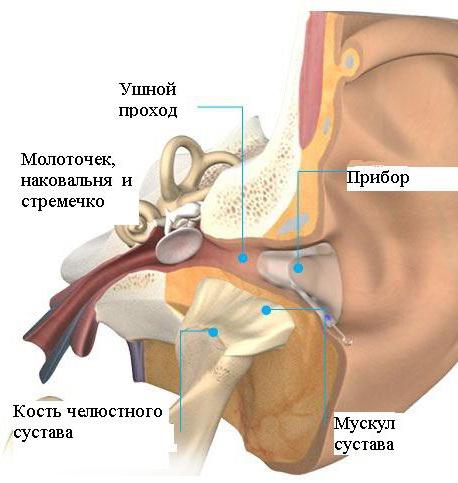
After all, the ear canal, its shell and jaw joint are in close proximity. Thus, osteomyelitis or meningitis can cause inflammation. It happens that this condition provokes lupus erythematosus (autoimmune disease) or rheumatoid arthritis. There are many options.
Symptoms of inflammation
The very first symptoms of this condition should not be ignored. A person will lose normal performance when his temporomandibular joint hurts. Inflammation, the symptoms of which we will cite, in medicine is called "arthritis of the temporomandibular joint." If inflammation is not treated, it leads to degenerative changes. This condition of the joint will already be called arthrosis. Then you will have to spend more time and money on treatment.

In acute and chronic arthritis, the symptoms vary. Symptoms in acute inflammation:
- redness and swelling in the joint;
- tissue hyperemia near;
- sometimes tinnitus and crunch;
- jaw grinding at night;
- difficulty opening your mouth;
- sharp pain when moving, extending to the ears and back of the head;
- dizziness;
- fever.
With chronic inflammation, other symptoms are:
- aching pain;
- feelings of jaw stiffness, especially if the sleeping position is chosen face down;
- the pain intensifies when you press the jaw;
- hearing loss is possible.
Usually, chronic inflammation is not accompanied by redness of the surrounding tissue or inability to open the mouth. However, it is still advisable to eat sparing liquid food at this time and treat inflammation. After all, prolonged inflammation without the necessary treatment will lead to facial deformation.
Infectious inflammation. Infection pathways
Inflammation of the jaw joint can also begin as a result of an infectious disease. Diseases such as tonsillitis, the common flu, can lead to inflammation of even the joints.
Also provocateurs can be:
- tuberculosis bacillus;
- syphilis virus;
- gonorrhea;
- mastoiditis (inflammation of the mastoid process of one of the bones of the skull);
- actinomycete fungus;
- purulent osteomyelitis.
In this case, together with the diagnosis of “inflammation of the temporomandibular joint” (symptoms are often eloquent), there will be no delay, with the determination of the type of infection, too. The therapist will determine the infection after collecting an anamnesis (medical history) and looking at the tests, and maybe asking for an X-ray. How can an infection get into the jaw joint?
An infection can switch and provoke inflammation of the jaw joint in several ways:
- through the blood;
- lymph
- directly through open cuts.
It is the underlying disease that needs to be treated. Since the joint structure itself is not damaged in this case, this problem will pass along with the cure of the infection.
Post-traumatic and rheumatoid inflammation
Those people who suffer from arthritis of the joints in the knees and elbows sometimes suffer from rheumatism of the jaw joint. Then you need to contact only a rheumatologist.
Arthritis after a trauma to the jaw will pass when the consequences of the trauma pass. Inflammation is triggered by blood clots that have fallen into the joint cavity. The doctor must clean the entire joint.
During acute pain, the jaw should be tightly bandaged and the patient should not be allowed to speak or chew. You will only have to eat liquid yoghurts and soups wiped on a blender at this time.
Joint inflammation as a result of malocclusion
At the beginning of the article it is mentioned that malocclusion can lead to inflammation. Why does this happen? In the human body, symmetry is one of the main laws. The height of the teeth should be the same and they should fit tightly together. Otherwise, the load on the joints will be uneven. In cases where the bite is not formed correctly: the lower jaw sags too much or protrudes, the jaw joint begins to hurt from the load over the years and can become inflamed. The same situation occurs when several teeth on one side are not enough and the load when chewing passes to the other side.
To cope with such pain, you need to contact the orthodontist who is involved in correcting such problems with the teeth. But it is necessary to exclude other causes of inflammation before starting treatment.
To check whether there are improvements or not, it is enough to put a special mouthpiece in your mouth and walk with it for several days. The pain will decrease or even disappear if the cause is really dental problems.
Complications of inflammation of the heart
An untreated disease of an infectious nature is one of the most dangerous causes of inflammation of the facial joint. What will happen if the joint is not treated? Firstly, pain will periodically come. Articular cartilage consists of connective tissue. And if suppuration begins in the joint area, this cartilage will quickly collapse.
A purulent temporal phlegmon comes. Then, if the patient does not come to the surgeon to remove pus, he can be transferred to other nearby tissues.
The acute nature of the disease without pus can also significantly spoil the life of someone who is afraid of treatment. The joint process begins in the joint, and over time it ceases to be mobile. This process is called fibrotic ankylosis. If this happens on one side, then the whole face is deformed. The next stage of the disorder is bone ankylosis, when the joint tissue finally ossifies.
How to deal with pain?
Sometimes pain due to arthritis of the facial joint is unbearable. People cannot eat for weeks, much less yawn. And while the main treatment lasts, you need to somehow cope with the pain that radiates far from the site of inflammation. Conventional drugs such as Ibuprofen are suitable for this. Any non-steroidal anti-inflammatory tablets available in a home medicine cabinet will come in handy.
During severe pain, the joint must be immobilized - apply a special bandage. It is advisable to apply a hot and dry compress to the temple. In a frying pan, it is enough to heat the salt and put it in a bag of simple fabric. Some people prefer to use ointments.
But it happens that tablets for pain relief are not enough. Then the doctor has the right to prescribe injections.
Such injections block the pain completely after 15 minutes. Assign in injections "Tramadol" or "Trimeperidine." These drugs belong to the class of narcotic drugs and are used by their doctor only in exceptional cases when the pain is unbearable, for example, after a jaw injury.
There is also a medicine "Nalbufin". The drug is not so strong, it does not apply to narcotic drugs, but it is not well understood.
Inflammation of the jaw joint. Treatment
How to determine inflammation of the jaw joint? Which doctor will help you find a solution to the problem? First you need to contact the therapist who will conduct the initial examination, and then he will refer to the specialist who can help practically.
If the patient has problems with a bite, you need to contact the dentist, otitis media should treat ENT. You may need the help of a gnatologist or a neuromuscular dentist. And if the pain began after an injury, then you need to go to the maxillary surgeon.
When the chewing process and opening the mouth becomes too painful, a person very often does not know which doctor should be consulted for these symptoms. Several pathologies can cause this pathology:
- dental nature;
- neurological properties;
- subject to surgical treatment;
- vascular.
The main pathologies will be various changes in the teeth and gums, lesions of the facial nerve, traumatic pathologies of the jaw or its joints.
In some cases, chewing will be painful for earaches due to inflammation.
Traumatic jaw lesions
Changes in the jaw caused by injuries can vary in severity:
- Bruises are the easiest injury options. Only soft tissues suffer, bones are not damaged. At the site of the injury, a bruise and swelling form on the face, they are accompanied by severe pain during movement of the jaws and chewing. Passes after the swelling and bruising subside, usually 7 days, if the pain is very severe, an X-ray should be taken to diagnose fractures of the jaw bones.
- Fracture is always the result of a blow or bruise. The injury is quite serious and very painful, swelling appears at the site of contact, a hematoma occurs after a short time. With bruises of the lower jaw, the patient cannot open and close his mouth. In case of damage to the bones of the upper jaw, hematomas may appear in the infraorbital region, sometimes such signs report a fracture of the base of the skull, with especially severe injuries, yellowish fluid is released, blood flows from the ear holes. With such injuries, a surgeon's consultation and x-ray examination must be carried out. Such injuries are subject to surgical treatment. Particularly severe fractures are subject to inpatient treatment.
- When trying to abruptly open the mouth or hit hard on one side, a lower jaw dislocation is possible in people with inflammatory joint pathologies. With such a lesion, acute pain is felt, the jaw rises in an unnatural position - it extends or twists, the mouth does not close, the patient cannot talk and explain what happened. The surgeon adjusts the jaw, after which an x-ray is performed to diagnose a fracture.
- A long-term consequence of the injury is aching pain, which is caused by damage to the gums and tooth fragments with an orthopedic fixative splint during a fracture. Fracture therapy is a fairly lengthy procedure, often requiring inpatient treatment.
Dental pathology
 Pathologies that will cause pain in the jaw when chewing are:
Pathologies that will cause pain in the jaw when chewing are:
- carious tooth pathologies, in which they are destroyed, painful pathological cavities are formed, nerve endings are constantly irritated;
- pulpitis, destroying dental tissue and affecting the nerve endings of the tooth;
- periodontitis - inflammation of the teeth;
- abscess in the periodontal region - an abscess that occurs in the oral cavity, near the teeth;
- osteomyelitis of individual sections of the jaw - inflammatory pathologies of bone tissue, are a complication of caries and pulpitis;
- dental lesions - splits of teeth, dislocations, fractures of the tooth neck.
- toothaches of uncertain origin;
- gingivitis - inflammation of the mucous membrane of the gums, in which they swell and redden. When the jaws are closed, pain is provoked by pieces of food that irritate them;
- inflammation of the tooth hole that occurs after tooth extraction with swelling and redness of the hole.
These pains in the jaws are sharp, throbbing, tend to intensify at night. The triggering factor will be the load on the jaw when chewing, strong adhesion of the jaw, the effect of too hot or too cold food.
The dentist and surgeon are involved in the therapy, an X-ray examination is carried out for diagnosis, antibiotic therapy is needed for osteomyelitis.
Neurological pain
The causes of severe pain in the jaw are also lesions of nerve nodes:
- trigeminal neuralgia cause very severe pain in the jaw with pathologies of its lower part. Type of pain - sharp, strong, appearing mainly at night, has a one-sided character, does not extend to the area located behind the jaw;
- pathologies of the upper nerve of the larynx, causing severe pain when chewing food and wide opening of the mouth, blowing your nose or sneezing, radiation to the chest is possible;
- inflammation of the glossopharyngeal nerve is quite rare.
Chewing pain. Additional symptoms will be pain during a conversation, drying out of the mucous membranes in the mouth. To stop the attacks, anesthesia is prescribed, drugs to relieve inflammation, with severe pain - surgical treatment is used.
Vascular lesions
The cause of pain in the jaw when opening the mouth and chewing can be vascular lesions:
- inflammation of the facial artery causes severe burning pains that are localized either along the edge of the lower jaw from the corner to the chin, or the upper in the nose. Sometimes the pain radiates to the region of the eye cavity;
- lesions of the carotid artery are now attributed to the causes of migraine. Pain can affect half of the face, half of the jaw, teeth, give in the ear. For treatment, medications are used.
Articular Disorders
 Pain in the jaw when chewing, tight adhesion of the jaws occurs with a state of joint dysfunction of the lower jaw. The cause of the violation may be:
Pain in the jaw when chewing, tight adhesion of the jaws occurs with a state of joint dysfunction of the lower jaw. The cause of the violation may be:
- injury;
- inflammatory process;
- malocclusion;
- injuries of chewing muscles.
Pain characteristically responds to the facial and temporal region, when you chew and open your mouth clicks are heard, the movements of the jaw are often limited.
Diagnostic method is radiographic examination.
Pain in the jaw joint is a common cause of seeking help from patients. It is due to a number of causes of changes in the temporomandibular joint (TMJ). In general, there is no single classification that all doctors use.
In our country, the classification presented by Sysolyatin and Ilyin is widely used. They subdivide all TMJ diseases into 2 groups: articular, that is, their own joint damage, and nonarticular, in which the muscle apparatus is affected.
Anatomy
Before studying the causes of pain, you need to know the anatomy of the TMJ. It is formed by the temporal and mandibular bones. Additional elements of the joint include: articular ligaments, articular tubercle, capsule and disk.
TMJ has its own functional specifics. The mobility of the lower jaw allows you to provide such vital functions as chewing, swallowing and speech formation. The presence of motor dysfunction or pain makes it difficult, and in some cases makes eating impossible. The lower jaw moves in three directions:
- vertical (down, up);
- sagittal (forward, backward);
- transversal (lateral)
Symptoms of a TMJ lesion
The main symptoms of TMJ joint diseases are clicks in the joint when opening and closing the mouth, limiting the opening of the mouth and pain in the temporal region, near the ear. In most cases, clicks in the TMJ are due to movement of the articular disc, and a crunch or sensation of sand in the TMJ appears due to uneven articular surfaces, which often develops with osteoarthritis. Joint pain is caused by an inflammatory process in the joint or periarticular tissues or muscle spasm. Let's move on to nosological diseases of the TMJ.
Arthritis
Arthritis is an inflammatory disease of the TMJ. They have various causes of development: traumatic, infectious and, in severe cases, systemic. According to the course, they are divided into acute and chronic, according to pathogens, into specific and non-specific.
Patients complain of local pain in the joint, near the ear, there are signs of movement restriction. Pain is also noted with palpation and pressure on the joint. With a rheumatic nature, the origin in patients in the morning is often a limitation of the opening of the mouth, which leaves during the day. If this symptom is detected, you should not delay with an appeal to a rheumatologist. In most cases, aseptic inflammation develops due to acute or chronic trauma. Chronic injury occurs when the posterior dentition is incorrectly positioned or when the disc is dislocated.
Sometimes, as already noted, the inflammatory process can go from the middle ear to the TMJ. This nature of the development and course of the disease leads to serious consequences in the form of secondary degenerative changes in the joint.
The treatment of inflammatory changes boils down to taking non-steroidal anti-inflammatory drugs and physiotherapeutic procedures. Of physiotherapy, UHF therapy, phonophoresis with hydrocortisone is preferable. In acute purulent inflammation, surgical treatment is performed. All patients are prescribed a sparing mechanical diet, restriction of opening the mouth.
Internal violations
Internal disturbances arise due to improper positioning of the internal elements of the joint. The main mechanism of development is considered the hypertonicity of the pterygoid muscles and the posterior extra-articular ligaments, which pull the articular disc. As a result, the disc shifts from the head of the lower jaw, and when you open your mouth or chew you hear a click near the ear. This defect occurs with functional occlusion, when the posterior dentition is abnormal or due to stressful situations and neuroendocrine disorders. 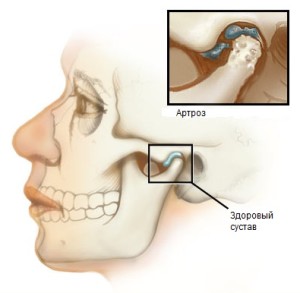
Most patients do not complain for a long time. Only loud clicks make you attract attention. The chronic course of the corrected anterior dislocation of the articular disc can lead to secondary degenerative changes in the head of the lower jaw. Usually pressure does not cause pain, but if synovitis is attached to the dislocation, then pain near the ear is added. The treatment of such dislocations is reduced to eliminating the causes of functional occlusion and muscle tone. With the development of synovitis, treatment is used as for arthritis.
Arthrosis
Arthrosis develops as the last stage of TMJ changes. As a result of constant microtrauma, the balance between the pressure on the joint and its physiological exposure is disturbed. There are two types of osteoarthrosis: sclerosis and deforming. The first develops in older people. Deforming arthrosis is characterized by various on the surface of the cartilage, detected only by x-ray methods.
Patients complain of restriction of movements on the affected side, movements lose smoothness, become step-like. The pain spreads to the ear and eyes, there is a headache, hearing loss. The diagnosis is made on the basis of an x-ray or linear tomography. It is very difficult. With degenerative changes in the joint, chondroprotectors, drugs that improve local blood circulation are prescribed. In the case of ineffective conservative therapy, severe pain and limited movement in the joint, surgical treatment is recommended.
Bruxism
Bruxism is a gnashing of teeth at night. The reason for its development is not specified. Its main mechanism is the parafunctional activity of the masticatory muscles of the mouth. In most cases, bruxism does not lead to. But if it provokes the appearance of pain in the temporal region and near the ear, treatment should be aimed at controlling the parafunctional activity of the muscles of the mouth. First of all, enamel suffers during gnashing of teeth, and the dentist's task is to prevent damage to tooth enamel. The main treatment is a doctor neurologist, neuropsychiatrist.
